European dermatology guidelines lay out consistent steps to improve management of dermatitis herpetiformis
By Amy Ratner, Director Scientific Affairs
Dermatitis herpetiformis (DH) affects about 10 to 25 percent of those who have celiac disease, though some evidence suggests that number is decreasing.
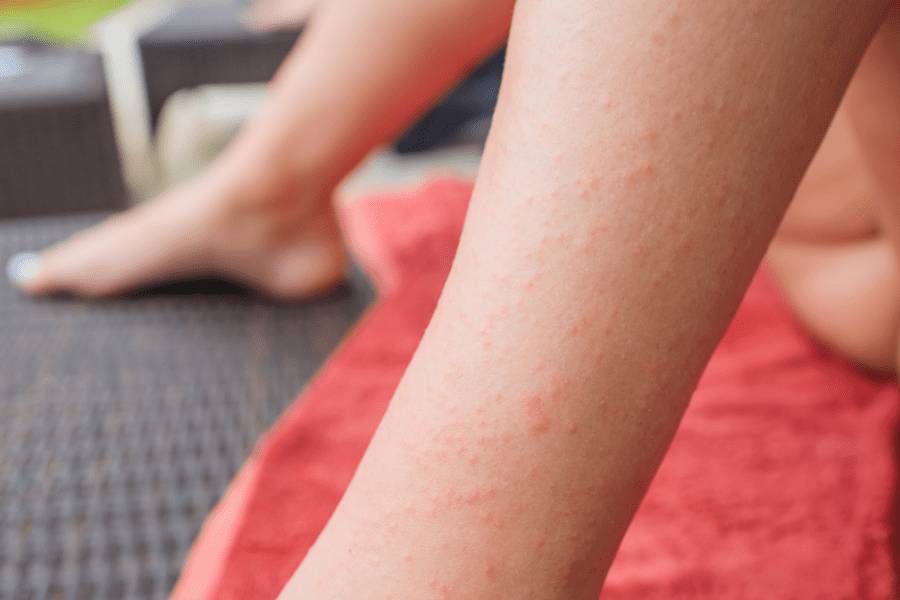
But the maddeningly itchy rash that is the hallmark sign of this skin manifestation of celiac disease can severely impact those who have it. In addition to the rash, many people with DH have the intestinal damage found in celiac disease. DH treatment includes a lifelong gluten-free diet.
Recently, the European Academy of Dermatology and Venereology compiled guidelines to support dermatologists in diagnosis and treatment of DH and improve the quality of management for patients. Researchers representing 13 European countries developed the guidelines, published in the Journal of the European Academy of Dermatology and Venereology, using evidence-based and expert recommendations. Guideline authors noted that previously there has been no European consensus about the management of DH.
The guidelines call for diagnosis to be made using medical history, a physical exam, a biopsy of the skin lesion, microscopic examination and direct immunofluorescence (DIF) microscopy of a biopsy of unaffected skin tissue, blood tests and a gastrointestinal assessment.
DIF is a technique that targets abnormal deposits of protein in a tissue sample. The staining patterns seen in tissue samples may be specific to a disease entity or they may need to be interpreted with the clinical and histological findings, the guidelines say.
In the case of DH, DIF microscopy is the gold-standard laboratory procedure for diagnosis, according to the guidelines. “It is necessary to perform [DIF] in any individual suspected to have DH,” the authors wrote.
Medical history and examination should include details about skin lesions and symptoms, as well as any gastrointestinal symptoms, including chronic or relapsing abdominal pain, diarrhea, constipation, weight loss and bloating, along with signs malabsorption and celiac disease. Also of interest would be any history of autoimmune diseases, in particular Hashimoto’s thyroiditis, insulin-dependent diabetes and pernicious anemia.
Blood tests for antitissue transglutaminase antibodies are recommended as part of diagnosis. Guideline authors note that TTG-IgA antibodies are specific markers for DH. An alternative is indirect immunofluorescence microscopy to detect endomysial antibodies, according to the guidelines.
In addition to the skin biopsies, the guidelines recommend a biopsy of the intestine to evaluate the degree of damage there, with at least four samples taken from different sections. In children TTG blood test results greater than 10 times the upper limit of normal, confirmed with a positive EMA test from a separate blood sample, would eliminate the need for a biopsy, in keeping with European Society for Pediatric Gastroenterology, Hepatology and Nutrition guidelines for celiac disease diagnosis in children. DH can occur in children, but it is uncommon.
Under the guidelines, in cases where DIF microscopy is repeatedly negative, but symptoms are typical of DH, a diagnosis can be made when a combination of the following criteria are met: there are lesions on the skin typical of DH with subepidermal vesicles and blisters; blood tests that detect TTG antibodies are positive; an intestinal biopsy indicates celiac disease; the genes related to celiac disease are present’ an iodine patch test or oral iodine challenge is positive; there is a response to dapsone treatment in one week; and there is response to a long-term gluten-free diet.
A lifelong gluten-free diet is the main treatment for DH, with dapsone prescribed initially to treat the itchy rash if it is severe and the symptoms it causes are intolerable to a patient, the guidelines say. Dapsone can also be prescribed if the gluten-free diet does not clear up the rash.
The skin responds more slowly to the gluten-free diet. It takes an average of two years for the rash to clear up when the gluten-free diet is the sole treatments, the guidelines note.
“The most efficient drug for symptomatic treatment is dapsone,” the authors wrote, noting that its effect can be observed within four days. This swift response to the drug supports the diagnosis of DH, according to the guidelines. Several other options exist for treating the rash itself, including sulfasalazine, potent topical corticosteroids, and antihistamines, but the alternatives are recommended only when dapsone is not tolerated or a patient refuses it as a treatment.
A strict gluten-free diet helps to reduce the dose of dapsone rapidly, and in most patients dapsone can be discontinued, the guidelines say. Patients should also be monitored for potentially serious side effects from the drug, including lowered red and white blood cell counts.
In the United States, the National Institutes of Health outlines some steps in the diagnosis and treatment of DH, but official guidelines are not readily available. Most advice for physicians and patients about diagnosis and treatment comes from celiac disease experts and centers. The European Society for the Study of Celiac Disease guidelines for diagnosis and treatment of celiac disease also includes DH recommendations.
Several recent studies by researchers from Italy align with the European DH guidelines. One 2019 study suggests that the incidence of DH is decreasing, potentially due to early recognition of celiac disease that does not allow enough time for DH to develop. That study also notes that misdiagnosis of DH is common with long delays in correct diagnosis, in part because it is a relatively rare condition.
You can read the DH guidelines here.
Opt-in to stay up-to-date on the latest news.
Yes, I want to advance research No, I'd prefer not to