Survey of people with celiac disease and non-celiac gluten sensitivity finds 90 percent have brain fog.

By Kate Avery, Director of Research and Patient Engagement
Brain fog is a symptom that gets a lot of attention in the celiac disease and non-celiac gluten sensitivity (NCGS) communities, but not as much attention from researchers. A survey conducted by Beyond Celiac asked 1,400 people with celiac disease and NCGS about their experiences with brain fog, including what their brain fog was like, how quickly it starts, and how long it lasts. This research was done in collaboration with researchers from Northeastern University and Beth Israel Deaconess Medical Center and was recently published in the Journal of Clinical Gastroenterology.
90 percent of survey participants (89% of celiac disease and 95% of NCGS) reported having brain fog. Participants were asked to choose from the following options to describe their brain fog: difficulty concentrating, forgetfulness, grogginess, detached, and mental confusion. Participants could also choose to provide their own description of their brain fog.
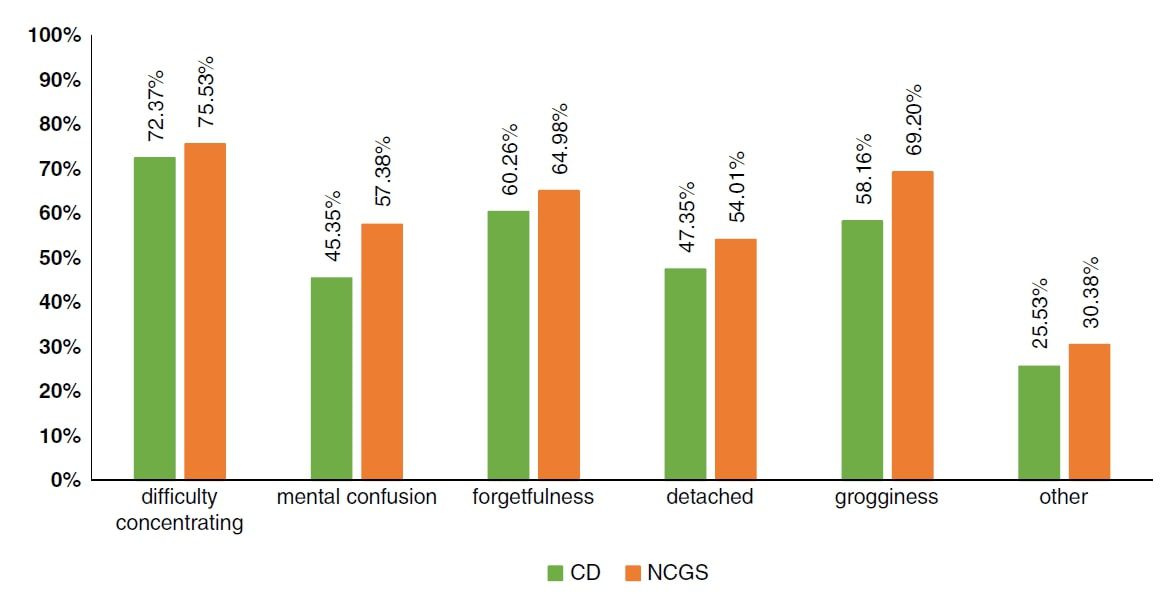
Participants with NCGS and celiac disease did not differ significantly in their responses. The most commonly-chosen descriptors of brain fog were difficulty concentrating, forgetfulness, and grogginess. The graph below shows the percentage of each participant type who chose each brain fog descriptor. These descriptors may help healthcare providers recognize that patients who use these words to describe symptoms may be experiencing brain fog.
Brain fog starts most often between 30 minutes to 1 hour after ingesting gluten in both celiac disease (20.6%) and NCGS (23.0%) participants. The majority of participants reported their symptoms peaked in the first 24 hours after eating gluten (58.6% of participants with celiac disease, 72.5% of participants with NCGS). 26.7% of participants with celiac disease and 30.4% with NCGS reported their brain fog symptoms lasted 1–2 days, and 20.3% with celiac disease and 24.5% with NCGS reported symptoms lasting 3–5 days. The researchers note this “suggest[s] a potential significant impact on activities including work and school.”
Over 500 participants chose to describe their brain fog in an open-ended answer. These open-ended answers were coded by themes. The most common themes were references to how brain fog impacted cognitive, physical, and psychological health as well as their quality of life. Cognitive impact and quality of life were found to be correlated in the analysis, suggesting the two are related. These themes may help healthcare providers better understand the many potential effects of brain fog. A poster presentation of these analyses was presented at the International Celiac Disease Symposium in 2019.
The researchers note this is a self-selected group of survey participants, so it cannot be used to determine the true rate of brain fog among all people with celiac disease and NCGS. However, it does suggest brain fog is common among people with these conditions and should be assessed as part of routine follow-up care, as well as included in patient-reported outcomes measures assessed in clinical trials. More research on the impact of brain fog on daily activities at work, school, and elsewhere is needed.
An abstract of the full publication is available here. If you would like a full copy of the article, email Kate Avery, Beyond Celiac Director of Research & Patient Engagement.