Celiac disease patients report they experience more than just GI symptoms, growing dissatisfaction with the gluten-free diet as a sufficient treatment

Beyond Celiac is taking the lead in presenting the patient perspective on celiac disease symptoms and the dissatisfaction with the gluten-free diet at an international meeting of celiac disease researchers and physicians in Sorrento, Italy.
Two posters based on data gathered by Beyond Celiac directly from those who have celiac disease are being presented by Alice Bast, chief executive officer, at the International Celiac Disease Symposium.
 One poster shows that those with celiac disease report having more than just gastrointestinal symptoms when they are exposed to gluten and the other that there is growing dissatisfaction with the gluten-free diet as a sufficient treatment.
One poster shows that those with celiac disease report having more than just gastrointestinal symptoms when they are exposed to gluten and the other that there is growing dissatisfaction with the gluten-free diet as a sufficient treatment.
Additionally, scientists whose research is being funded by Beyond Celiac are also presenting at ICDS. Michael Fitzpatrick, MD, of the University of Oxford, is giving an oral presentation on the investigation into the pathogenic role of so-called killer T-cells in celiac disease, work funded through the 2019 Beyond Celiac Established Investigator Award.
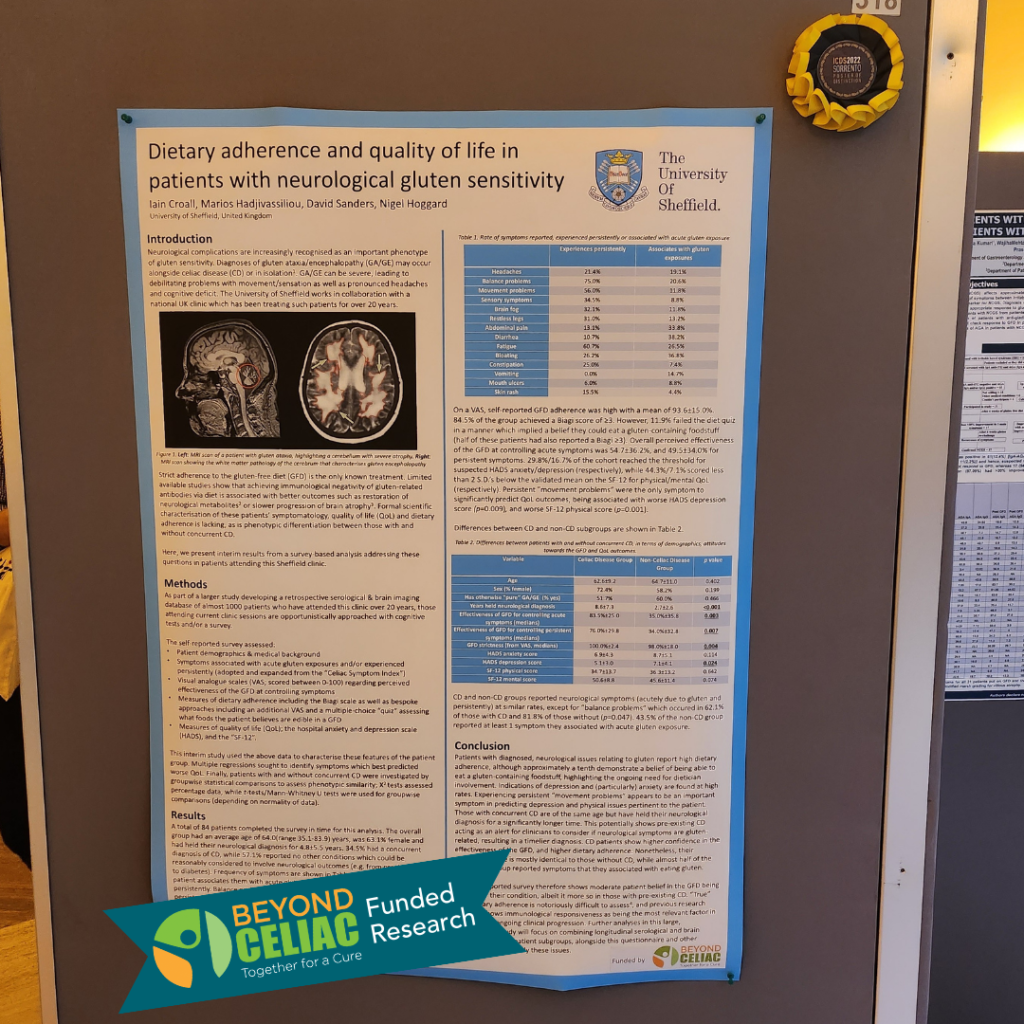 Iain Croall, PhD, of Sheffield University, is presenting a poster on early findings from research into the neurological and neuropsychological manifestations of celiac disease and gluten-related disorders. This work was funded by the 2021 Beyond Celiac Established Investigator Award.
Iain Croall, PhD, of Sheffield University, is presenting a poster on early findings from research into the neurological and neuropsychological manifestations of celiac disease and gluten-related disorders. This work was funded by the 2021 Beyond Celiac Established Investigator Award.
The Beyond Celiac symptoms poster is based on an online survey taken by more than 2,200 adult participants registered in the Go Beyond Celiac patient registry. About 98 percent of the 2,000 symptomatic participants reported having gastrointestinal symptoms and about 96 percent reported non-gastrointestinal symptoms, the poster shows.
The most common gastrointestinal symptoms were abdominal pain or discomfort, abdominal bloating, gas, and diarrhea. The most common non-gastrointestinal symptoms were brain fog, fatigue, irritability, and headaches. Most participants with symptoms reported a combination of gastrointestinal and other symptoms.
“Physicians should be aware of common non-GI symptoms when considering diagnostic screening or celiac disease management,” according to authors of the poster.
The second poster, based on two community surveys taken by Beyond Celiac eight years apart, shows that celiac disease patient attitudes about the gluten-free diet have shifted significantly in the last decade.
Survey participants who agreed “a great deal” that the gluten-free diet is an adequate treatment has decreased by more than half. In 2014, of the 1460 survey participants, about 27 percent agreed compared to about 12 percent of the 1140 who answered the survey in 2022. Meanwhile, the proportion of participants who agreed “not at all” that the gluten-free diet was a sufficient treatment increased from about 13 percent in 2014 to about 23 percent in 2022.
“Beyond Celiac is playing a vital role in educating the celiac disease community, physicians and researchers about challenges posed by inadvertent gluten exposure, the burden of the disease, and the need for treatments beyond the diet,” notes Beyond Celiac Director of Research and Patient Engagement Kate Avery, MPH, who is an author on both Beyond Celiac posters.
Meanwhile, the poster being presented by Croall is based on the survey response of 84 patients treated at Sheffield for neurological conditions who were asked to report symptoms associated with acute gluten exposures and/or symptoms they persistently experience. Overall, survey participants ranked the gluten-free diet as being moderately successful in controlling their symptoms.
Those surveyed had gluten ataxia/encephalopathy with and without a diagnosis of celiac disease. Survey participants also reported on quality of life and how well they followed the gluten-free diet, with both groups reporting high adherence.
Both groups also reported similar rates of neurological symptoms that occurred acutely and persistently. Balance problems were an exception, occurring in about 60 percent of those with celiac disease and about 80 percent of those who don’t have celiac disease.
Overall, the perceived effectiveness of the gluten-free diet in controlling acute symptoms was about 55 percent compared to 50 percent for persistent symptoms. “Indications of depression and particularly anxiety are found at high rates, the poster concludes. “Experiencing persistent “movement problems” appears to be an important symptom in predicting depression and physical issues pertinent to the patient,” according to the poster authors.
The survey is part of the larger study developing a retrospective blood test sample and brain imaging database of almost 1,000 patients who have been seen at Sheffield over 20 years.
ICDS, which takes place every other year in a different country around the world, is forum where scientists, clinicians, health allied professionals, patients associations and industry meet to exchange knowledge and experience and to foster cooperation, according to ICDS organizers.
Celiac disease is a serious autoimmune condition. The disease causes damage to the small intestine, resulting in debilitating symptoms, and if left untreated can lead to a number of serious, long-term health problems including brain damage, infertility and some types of cancer. Celiac disease affects one in 133 Americans.
Opt-in to stay up-to-date on the latest news.
Yes, I want to advance research No, I'd prefer not to