Have you been glutened?
April 12, 2017
An at-home pregnancy-like test may soon be available to give you the answer
![]()
By Amy Ratner, Medical and Science News Analyst
Over-the-counter tests that detect gluten in stool or urine could be on store shelves in the United States by the end of the year.
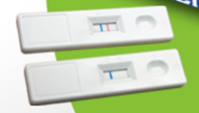
Called GlutenDetect, they work like a pregnancy test with a stick that shows a positive or negative result when a sample of urine or stool is applied to one end. The at-home tests will offer consumers a quick and easy way to determine if they’ve been exposed to gluten, the protein that can trigger symptoms and intestinal damage in celiac disease patients and cause problems for gluten sensitive patients as well.
A version of the test that measures the amount of gluten consumed and gives a numerical result could also be available by the end of the year, according to the company distributing the tests, but it would have to be sent to a central laboratory for analysis.
 Physicians could use both the quick-read test in the office and also results from the lab-analyzed test to help patients manage celiac disease or gluten sensitivity by determining whether gluten is getting into the gluten-free diet and to explain why symptoms are occurring or blood test results are not normal.
Physicians could use both the quick-read test in the office and also results from the lab-analyzed test to help patients manage celiac disease or gluten sensitivity by determining whether gluten is getting into the gluten-free diet and to explain why symptoms are occurring or blood test results are not normal.
The tests will also have important implications for researchers working on experimental celiac disease treatments. These scientists need a reliable way to measure how much gluten patients are consuming as part of the process of proving that a drug can protect against its harmful effects.
When the Food and Drug Administration (FDA) recently weighed in on what is needed for approval of any drug to treat celiac disease, the agency noted that a reliable method of monitoring gluten exposure will be key. A test that could measure gluten and meet this critical unmet need could help speed new treatments.
The tests were developed by Biomedal, a Spanish company that has already launched the laboratory version in Europe and will begin offering the over-the-counter test in Barcelona in June. GlutenDetect is being distributed in the United States by Glutenostics, a California-based company, which intends to sell them in stores and online.
Though an exact price has not been set, it’s likely to be similar to over-the-counter pregnancy tests at $15 to $20 for a one-time use test.
A guessing game
One of the toughest questions facing celiac disease patients, their doctors, dietitians and scientists studying the condition is how to measure how much gluten someone on the gluten-free diet has been exposed to.
For patients, especially those who tend to have obvious symptoms, it’s a constant guessing game. Did the restaurant meal they ate the night before come into contact with gluten? Are the symptoms they experience after the meal related to gluten, a different food sensitivity or even food poisoning? Does one of the gluten-free foods in their pantry contain some harmful amount of gluten?
For doctors and dietitians, there’s the frustration of not being able to offer much help beyond the general recommendation that celiac disease patients follow the gluten-free diet. What do they say to a patient who is trying to do just that but continues to have symptoms?
For researchers, it’s a challenge to know for certain whether patients who participate in clinical trials are accurately reporting whether they are eating gluten. How can they be sure their study results reflect the reality of the interaction between gluten consumption and, for example, a drug to protect against it?
Francisco Leon, M.D., Ph.D., a founder of Glutenostics and partner in Biomedal, says the company is working on different versions of the urine and stool tests to address these issues. However, the test will not be specifically aimed at those with celiac disease or gluten sensitivity.
“Following regulations and because the test is not FDA approved, the over-the-counter product will not be marketed to any specific population and will not make any claim other than whether or not there is gluten found,” Dr. Leon says. “It will be offered to anyone avoiding gluten to better manage their dietary habits.”
The majority of people avoiding gluten in the United States do not have celiac disease, he notes, pointing to a recent study published in the journal JAMA Internal Medicinethat found an estimated 1.76 million people have celiac disease, compared to 2.7 million people who adhere to a gluten-free diet even though they don’t. “Consequently, the at-home product will be marketed to the general population, while the lab test will be primarily used by celiac patients and their doctors,” he explains.
Approval of the tests under the FDA Food Drug and Cosmetic Act would require clinical trials conducted in the United States, which would delay getting GlutenDetect on the market for several years. Glutenostics may run these trials in the future, according to Dr. Leon, and seek FDA approval that would allow medical claims.
Researchers can use the more complex version of the test, an enzyme-linked immunosorbent assay also called ELISA, in the laboratory to analyze many samples at once and get precise numbers on the amount of gluten consumed by study participants.
The lab version of the stool test is already being used in clinical trials to monitor if participants have consumed gluten. The performance of the tests has been established in clinical studies in Europe, and is expected to be replicated soon in the United States in collaboration with leading academic experts, according to the Glutenostics.
Use of the tests
The urine test for at-home use would give a simple positive or negative result based on whether someone has consumed more than 25 to 50 milligrams of gluten within the previous two to 24 hours. Meanwhile, the stool test detects similar levels of gluten consumption from two to four days after it has occurred.
Fifty milligrams of gluten is the smallest amount known to cause intestinal damage in celiac disease, so any positive result would mean that potentially harmful gluten is being consumed. For celiac disease patients, the goal would be to keep getting negative results over time.
Although gluten is usually measured in parts per million (ppm) in the United States, including in FDA rules that limit the amount of gluten in a food labeled gluten-free to less than 20 ppms, the test results can’t be measured that way, according to Dr. Leon. He says parts per million calculates a relative amount of gluten dependent on the total amount in a food. GlutenDetect tallies the absolute, or total, amount of gluten independent of how much food is consumed.
“For patients, any positive result means you are getting gluten in your diet, at a level known to potentially make celiac patients sick,” Dr. Leon says. “That’s why we determined that a ‘yes’ or ‘no’ result would be useful to celiac disease patients and anyone avoiding gluten.”
The at-home version, called a lateral flow test, uses technology similar to a pregnancy test. A drop of urine or stool is mixed with a solution, called a buffer, and put on one side of the test strip. It diffuses and then reacts with an antibody located on the other side of the strip. The antibody then reacts with antigens in the sample and produces a positive or negative result.
The tests have also been compared to glucose monitoring strips used by those with diabetes and a scale for those watching their weight because they are tools that provide evidence that connect diet and health.
“Tools to detect gluten exposure have the potential to revolutionize the management of celiac disease,” says Jocelyn Silvester, M.D., director of research of the Celiac Disease Program at Boston Children’s Hospital. Dr. Silvester and colleagues recently published a study of gluten exposure that found celiac disease patients are frequently exposed to gluten even when they are trying to follow a strict gluten-free diet and often don’t realize it until symptoms occur.
She notes that a device to test for gluten would help patients who get a positive result know for certain that they’ve exposed, enabling them to more easily identify the source and avoid it in the future. Meanwhile, those who get a negative answer would have the reassurance that a food is safe, preventing them from unnecessarily restricting their diet. Additionally, Dr. Silvester says, the tests could pinpoint whether symptoms are due to gluten or some other cause.
Tricky, touchy subject
Gluten exposure and compliance with the gluten-free diet are tricky and touchy topics among those who have celiac disease. Currently, there is no easy and reliable method to determine whether and how much gluten a person has consumed.
Doctors and dietitians usually rely on the same blood test used to diagnose celiac disease, anti-tissue transglutaminase (tTG), to help patients manage the condition. But studies have shown that while the test is very effective at diagnosis, it doesn’t do a very good job in helping to monitor celiac disease, particularly since patients with negative blood test results often have intestinal damage that’s revealed only through an invasive biopsy.
Patients who are working hard to strictly follow the diet are often frustrated by how easy it is to unknowingly eat something that contains gluten, usually because of cross-contact. Products that appear to be gluten-free have sometimes come into contact with gluten-containing wheat, barley or rye or oats from a contaminated source. Dining out is challenging because food prepared in restaurants or otherwise outside the home presents a high-risk for cross-contact with gluten when it’s stored, prepared or served.
Consequently, those with celiac disease face uncertainty and anxiety when they think they’ve been exposed to gluten. Some have symptoms but aren’t sure of the timing or source of exposure, and others have minimal or no symptoms but still might have been exposed. Finally, some have symptoms but don’t recognize them as being related to celiac disease.
When researchers set up studies to test the effectiveness of drugs to treat celiac disease, it can be a challenge to accurately determine how much gluten a study participant has consumed. Currently, patient food diaries, the tTG test and follow-up biopsies are used, but there is a significant need for a better, less invasive method.
Complying with the diet
Gluten resists complete digestion in everyone, not just those who have celiac disease. This results in a significant fraction being excreted in urine and stool. Several studies sponsored by Biomedal have focused on this process.
Unlike other proteins, gluten proteins are not completely digested and remain in the gastrointestinal tract. A 2012 study published in the American Journal of Clinical Nutrition concluded that gluten peptides could be sensitively detected in human stool in positive correlation to the amount of gluten consumed.
Meanwhile, a study published in 2016 in the American Journal of Gastroenterology found limitations with traditional methods of monitoring the gluten-free diet among 188 celiac disease patients. Researchers found that nearly 30 percent had detectable levels of gluten immunogenic peptides (GIP) in their stool. However, neither tTG blood test results nor dietary questionnaires filled out by participants indicated gluten exposure.
The study found that about 18 percent were not compliant with the gluten-free diet based on the food questionnaire, compared to the nearly 30 percent designated as non-compliant according to the GIP results. More than 70 percent of those who had positive GIP tests had negative anti-tTG IgA results.
“Clinically, GIP analysis would allow celiac disease patients to detect unintentional gluten contamination and prevent the complications associated with untreated celiac disease,” the study says. Researchers note that because it is highly sensitive and noninvasive, the new tests could become the method of choice for physicians monitoring celiac disease patients.
“Based on the 70/30 data, it seems a large proportion of patients are exposed to gluten unknowingly and unintentionally,” Dr. Leon said. “This confirms what patients already know; that they try their best, and it’s often not enough.”
Detecting gluten
A 2015 study in the journal Gut found that as little as 25 to 50 milligrams of gluten in processed bread, which is approximately the amount that appears to be detrimental for most patients with celiac disease, can be detected in urine.
Recovery of measurable gluten peptides in urine indicates that it has been absorbed by the intestine, been circulated and filtered by the kidneys, according to the study.
“The method was sensitive, specific and simple enough to be convenient for clinical monitoring of patients with celiac disease, as well as for basic and clinical research applications, including drug development,” study authors wrote.
The study found that there was “poor correlation” between intestinal healing and blood test results, contrasting with “good correlation” between GIP in urine and intestinal damage.
Seventy-six healthy controls provided urine samples in which GIPs were detected four to six hours after a single gluten intake and remained detectable for one to two days. All showed gluten excretion in their urine. Among participants with celiac disease following a gluten-free diet, 48 percent of adults and 45 percent of children had detectable GIPs in their urine.
Researchers then looked at the intestinal biopsies of 25 celiac disease participants who were either GIP positive and negative. Those who were GIP negative showed little or no damage to the intestine, while six of the seven who were GIP positive had clear abnormalities.
Additionally, five participants who had severe intestinal damage had negative celiac disease blood tests, including tTG. Four who had lesser damage had positive blood test results. And reports of dietary history also did not line up with evidence of intestinal healing.
“This study indicated only the urine GIP detections correlated with compliance with the gluten-free diet and with mucosal healing in patients with celiac disease on a gluten-free diet,” the authors write. They note urine sampling is non-invasive, less expensive and offers easy collection, transport and storage. Patients are also familiar with urine tests as they commonly used to diagnose illnesses and conditions in the doctor’s office and over-the-counter.
“We have known for a long time that antibody blood tests (anti-tTG, anti-DGP) are not sensitive to smaller or shorter dietary exposures,” Dr. Leon says. “Many studies show that blood tests are negative in two-thirds of patients with mucosal atrophy. Consequently, there is a need for better biomarkers of celiac disease activity”.
Seven clinical research studies using the gluten and stool tests are currently going on around the world, including in the United States.
Dr. Silvester is among those using both tests in celiac disease research and has been impressed with the results. “These tests have many uses, including to screen for gluten exposure, which may prevent the need for intestinal biopsy,” she says. “Once a trial is underway, they can be used to monitor adherence to either the gluten-free diet or a gluten challenge.” Quantitative results that measure gluten exposure are particularly useful in clinical trials.
Window of opportunity
One of the key differences between the urine and stool tests is the window of opportunity each provides for measuring gluten.
The urine test has been shown in studies to be able to detect gluten from two to 24 hours after it has been consumed, though It’s most accurate within six to 18 hours. It could be used, for example, by celiac disease patients who eat out in a restaurant, have symptoms and want to confirm that they’ve been exposed to gluten. In practice, the test works best when urine is collected first thing in the morning after suspected exposure or if repeated several times during the day.
Additionally, patients who do not have symptoms but wonder if they are being exposed could use the test to check. “If the result is positive, it might require some dietary detective work to determine the source,” Dr. Leon says. “But it will help all those who are trying to avoid gluten improve their compliance with the gluten-free diet.”
With the stool test, GIP starts to appear after 48 hours and can be detected for two to four days, though it has been found in some patients’ samples up to seven days after consumption.
“If you have suspected gluten exposure and you want to know quickly at home, the urine test is best,” Dr. Leon says. “If you are going to the doctor a few days later, the urine test is not going to help and the stool test is the better choice.”
Physicians could use GlutenDetect in a variety of ways to help patients understand what is going on with their gluten-free diet.
In 15 minutes, a symptomatic patient could have positive tests results that tell them whether they are consuming gluten. Other times, a doctor who is following a patient through multiple visits could use the lab version to get quantitative results.
“For example, a patient who was initially found to have a high amount of GIP, but tests much lower on a later test would know he or she is improving,” Dr. Leon says. “But if the numbers are not coming down, you know the patient is struggling with the diet and may need further nutritional counselling.”
A current picture
He notes that one of the advantages of the tests is that they give patients and doctors a current picture of gluten exposure compared to the tTG test and biopsy, which show what has happened in the past few months. “You are looking at what’s happening today, and patients can review their diets,” he says. “This is a tool to help manage a gluten-free diet.”
The tests will work for anyone who wants to determine whether they are consuming gluten, including those who have gluten sensitivity. Among celiac disease patients, Dr. Leon expects those who have symptoms to be more likely to use the test than those who are symptom free.
He says asymptomatic patients would benefit more than some may realize because they often have the intestinal damage that can lead to complications. And for some asymptomatic patients there is a heightened level of anxiety caused by not knowing if they are being affected by gluten without symptoms as a clue.
Sam Master, M.D., a former member of the Beyond Celiac Patient and Family Advisory Council who is asymptomatic but still carefully reads labels after 14 years on the gluten-free diet, says he would very likely use a test to determine whether he has ingested gluten. “The underlying pathologies of an untreated autoimmune disease are what drive my self-control for diet adherence,” he says, noting that if he could determine that he was unknowingly being exposed to gluten he would want to reassess his diet and figure out where gluten was sneaking in.
“Most patients try their best to be gluten-free, but there is just not enough information,” Dr. Leon says. He points to the case of a gastroenterologist, who has been knowledgeable about celiac disease for a decade and was diagnosed himself three years ago. His blood test results are still positive despite his attempts to follow the diet. “He can’t figure out where he is getting the gluten.”
You can read more about GlutenDetect here. To keep up with further development of the tests and other research news, sign up for our Research Opt-in here.